Methods:
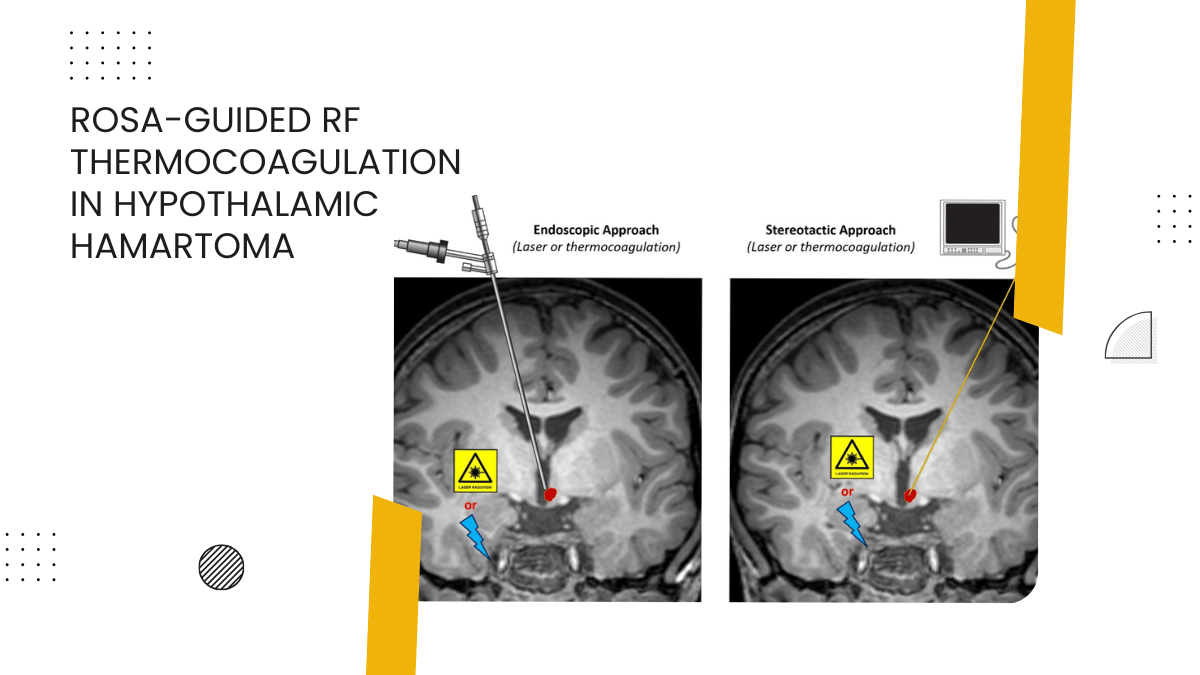
Five patients with HH and gelastic seizures underwent SRT. Robotic guidance (ROSA) was used for the placement of electrodes. An O-arm was used for coregistering and confirming the robotic trajectory with real-time intraoperative imaging. Intraoperative computed tomography was merged with preoperative magnetic resonance imaging to confirm the exact position and trajectory of the electrode. Ablation was performed using a radiofrequency generator (70°C for 60 seconds). Multiple target sites were ablated to achieve proper ablation and disconnection.
Results:
Most patients (4/5) had an International League Against Epilepsy class I outcome. One patient, 2 sittings of lesioning. All but 1 electrode could be placed in the planned trajectories. One electrode was detected to have a medial deviation, and it had to be revised. No permanent complication was observed.
Conclusions:
SRT is a cost-effective method of treating HH when compared with laser interstitial thermal therapy. With the use of a robotic arm we have demonstrated accurate placement of electrodes. Intraoperative computed tomography acquired using an O-arm can be merged with preoperative magnetic resonance imaging. This confirms electrode location and trajectory on a real-time basis by performing intraoperative imaging. This method is safe and can be used for radiofrequency ablation of HH.
Refer the link for more details: https://www.sciencedirect.com/science/article/abs/pii/S1878875018302365


Add a Comment