Degenerative spine disease is one of the most common conditions I treat in my practice, and over the years, I’ve seen how deeply it can affect a person’s daily life. As we grow older or sometimes even earlier due to lifestyle, genetics, or work-related stress, the structures in the spine begin to wear down. This natural degeneration can lead to pain, stiffness, nerve compression, reduced mobility and, in many cases, chronic discomfort.
One of my recent patients, Tina, a 35-year-old working professional, is a perfect example of how degenerative spine disease can affect even younger individuals. Despite maintaining an active lifestyle, she began experiencing persistent lower back pain that radiated down her legs. At first, she dismissed it as work stress or a bad sitting posture. But when the pain started interfering with her ability to sit, work and sleep comfortably, she decided to seek help. After a thorough evaluation, imaging studies and clinical assessment, she was diagnosed with early-stage spondylitis, a form of degenerative spine disease.
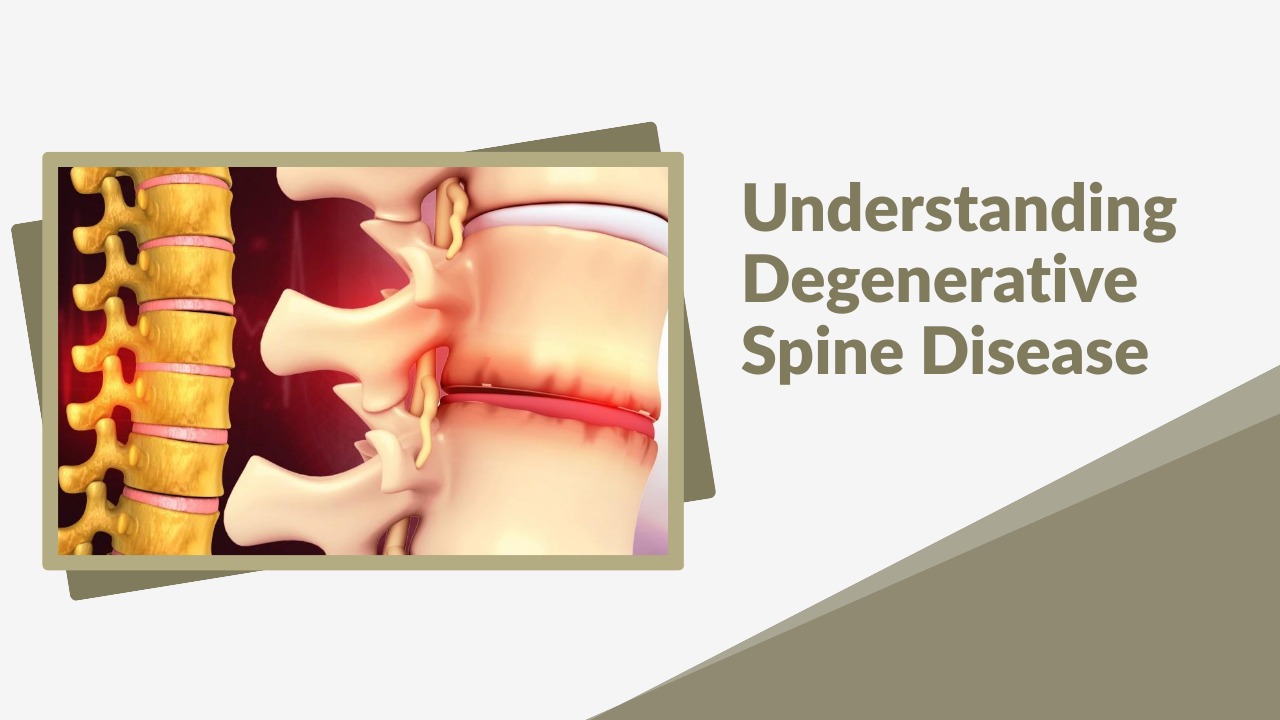
What Causes Degenerative Spine Disease?
The spine is made up of vertebrae, discs, joints and ligaments that work together to support movement. Over time, repeated mechanical stress causes the discs to lose water content, the joints to become arthritic and the ligaments to thicken. Factors such as sedentary lifestyle, obesity, genetics, smoking, improper posture, heavy lifting, and previous injuries accelerate this process. In patients like Tina, who spends long hours working at a desk, the constant strain on the spine contributes to early degeneration.
Symptoms You Should Never Ignore
Patients often report chronic back or neck pain, morning stiffness, radiating leg or arm pain, numbness, tingling, or weakness. Some develop difficulty walking long distances or performing daily tasks. In Tina’s case, her symptoms worsened over a few months, especially during prolonged sitting and bending forward. Early identification of these signs is crucial for preventing long-term damage.
How Degenerative Spine Disease Is Diagnosed
Diagnosis involves a detailed clinical examination, X-rays, MRI scans and occasionally CT imaging. These tests help identify disc degeneration, facet joint arthritis, nerve compression, spondylolisthesis or spinal canal narrowing. With Tina, her MRI clearly showed inflammatory changes and disc degeneration consistent with spondylitis, allowing us to create a personalised treatment plan.
Effective Treatment Options
The good news is that most patients improve without surgery. The treatment approach depends on the severity of symptoms and the extent of degeneration.
- Medications to reduce inflammation and pain
- Targeted physiotherapy to improve posture, strengthen core muscles and enhance spinal stability
- Lifestyle modifications, including ergonomic correction and weight management
- Heat therapy, bracing or guided exercises for symptom relief
- Image-guided injections in patients with severe inflammation or nerve compression
In Tina’s case, a structured rehabilitation program combined with medication and posture training helped her return to normal activities within weeks.
When Surgery Is Needed
Only a small percentage of patients require surgery, usually when there is severe nerve compression, spinal instability or progressive neurological deficits. Modern spine surgery techniques, including minimally invasive procedures, ensure faster recovery, reduced pain and better long-term outcomes.
Degenerative spine disease is common, but it is manageable with the right approach. My experience has shown that early diagnosis, timely treatment and lifestyle modifications can significantly improve quality of life. If you experience persistent back or neck pain like Tina, don’t ignore it, early evaluation can prevent long-term complications and restore a healthy, active life.
Add a Comment