As a pediatric pulmonologist, one of the most valuable tools in my practice is bronchoscopy. Over the years, I have seen how this procedure can be life-changing for children with chronic respiratory issues, recurrent infections, or suspected airway abnormalities. Through my experience, I’ve learned that while bronchoscopy may seem intimidating to parents, understanding the process, benefits, and safety measures can alleviate anxiety and help families make informed decisions. In this blog, I want to share what bronchoscopy is, what it diagnoses, how it is performed, the recovery process, possible complications, and the immense value it brings to pediatric care.
What is a Bronchoscopy?
A bronchoscopy is a medical procedure that allows doctors to look directly inside a child’s airways, including the trachea, bronchi, and smaller branches of the lungs. Using a thin, flexible tube equipped with a camera and light, we can visualize the airway in real-time and identify any abnormalities. In children, especially infants and toddlers, the airways are delicate, and even small obstructions or inflammation can significantly impact breathing. This is why bronchoscopy is such a critical diagnostic and therapeutic tool in pediatric pulmonology.
From my perspective, bronchoscopy is both an art and a science. While imaging studies such as X-rays or CT scans provide an overview, bronchoscopy offers a direct look at the airway. It is the only way to visually confirm conditions that can otherwise remain hidden, allowing us to intervene accurately and promptly.
What Does a Bronchoscopy Diagnose?
In my practice, bronchoscopy is used to diagnose a variety of conditions, ranging from common to complex:
1. Airway Obstructions: These may include mucus plugs, tumors, or congenital malformations. Children with persistent breathing difficulty often benefit from bronchoscopy to locate and sometimes remove these obstructions.
2. Chronic or Recurrent Infections: In cases of repeated lung infections, bronchoscopy allows us to collect samples directly from the airway for accurate microbiological analysis. This ensures that treatment is targeted and effective.
3. Foreign Body Aspiration: Young children frequently inhale small objects, which can lead to sudden respiratory distress. Bronchoscopy is the safest and most reliable method to locate and remove these foreign bodies.
4. Inflammatory or Allergic Conditions: Some children have chronic inflammation or airway hyperreactivity due to asthma or allergies. Bronchoscopy helps assess the severity and extent of airway involvement.
5. Congenital Abnormalities:*Structural problems such as tracheomalacia or bronchomalacia can be directly visualized during bronchoscopy, guiding further interventions.
Each child’s case is unique. I always emphasize to parents that bronchoscopy is not just a diagnostic tool, it is a bridge to precise, individualized treatment.
What Happens During a Bronchoscopy?
For children, the thought of a bronchoscopy can be scary for both parents and the patient. In my experience, careful preparation and clear communication help ease anxiety.
Before the procedure, the child undergoes a thorough pre-assessment, including a review of medical history, current medications, and any previous allergic reactions. In most cases, bronchoscopy is performed under sedation or general anesthesia to ensure that the child remains comfortable and still throughout the procedure. This also allows for safe and precise evaluation of delicate airways.
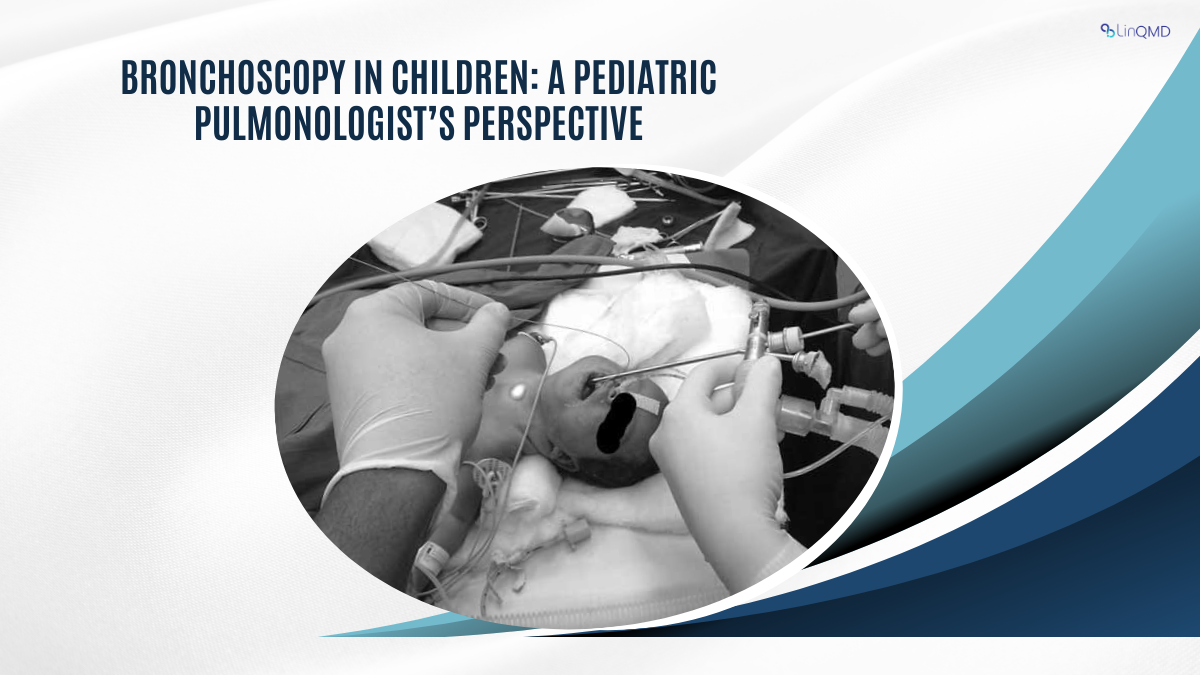
During the bronchoscopy, I gently insert the flexible bronchoscope through the nose or mouth, carefully advancing it into the trachea and bronchi. The camera transmits high-resolution images to a monitor, allowing me to identify inflammation, obstructions, or structural abnormalities. If needed, I can perform therapeutic interventions during the procedure, such as suctioning mucus plugs, removing foreign bodies, or collecting samples for laboratory testing.
Communication with parents during this process is critical. I make it a point to explain each step in simple terms beforehand, and reassure them that the child will be continuously monitored by a specialized anesthesia team. This approach not only reduces stress but also fosters trust, which is vital in pediatric care.
How Long is Recovery After a Bronchoscopy?
Recovery time after bronchoscopy depends on the child’s age, the type of sedation or anesthesia used, and whether any therapeutic procedures were performed during the bronchoscopy. In my experience:
- Most children recover within 2–4 hours after the procedure when performed under sedation.
- If general anesthesia is used, monitoring may be needed for a slightly longer period until the child is fully awake and stable.
- Mild throat discomfort, coughing, or hoarseness may persist for a few hours to a day, but these symptoms are usually temporary.
I always provide parents with detailed post-procedure instructions, including monitoring for fever, persistent coughing, or difficulty breathing, and I encourage them to reach out immediately if any concerning symptoms arise. In nearly all cases, children recover quickly and are able to resume normal activities within a day.
Possible Complications During a Bronchoscopy
Bronchoscopy is generally safe, especially when performed by an experienced pediatric pulmonologist in a fully equipped facility. However, like any medical procedure, it carries potential risks. In my practice, I take every precaution to minimize these complications. Some possible risks include:
- Bleeding: Minor bleeding can occur, especially if a biopsy is performed. It is usually self-limiting.
- Infection: The procedure is performed under sterile conditions, but there is a very small risk of introducing infection.
- Reaction to Sedation or Anesthesia: While rare, some children may have an adverse reaction, which is why continuous monitoring by an anesthesia team is essential.
- Airway Spasm or Collapse: Very rare, but can occur in children with hyperreactive airways; managed immediately by the critical care team.
In my experience, complications are uncommon, and when they do occur, prompt recognition and management ensure a safe outcome. Parents often express relief when they see how closely we monitor their child before, during, and after the procedure.
Conclusion
Bronchoscopy is more than a medical procedure, it is a window into a child’s airway and a tool for life-changing interventions. Over the years, I have seen children with chronic cough, recurrent infections, or airway obstructions regain normal breathing, improved health, and a better quality of life thanks to timely bronchoscopy.
Parents often come to me worried and anxious, but witnessing their child recover and thrive is the most rewarding aspect of my practice. Bronchoscopy allows us to diagnose accurately, treat effectively, and prevent long-term complications. As a pediatric pulmonologist, I consider it both a privilege and a responsibility to use this powerful tool to help children breathe easier, live healthier, and grow stronger.
Every child is different, every airway tells a story, and every procedure reminds me why I chose this specialty: to combine advanced medical care with compassion, precision, and hope. Bronchoscopy is not just a procedure; it is a bridge between uncertainty and healing, and I feel honored to guide families through that journey.


Add a Comment