Spinal problems are common in older adults, but hearing terms like “scoliosis” or “degenerative spine disease” can feel worrying. Many patients ask: “Does this mean I will lose mobility or need surgery?” I want to share a real-world example (with details changed for privacy) to explain how modern care can improve pain, posture, and quality of life — even for someone in their seventies.
The patient:
Mrs. X is a 75-year-old retired teacher who had been struggling with back pain for several years. She noticed:
- Increasing discomfort in her lower back
- Stiffness that limited bending and household activities
- Reduced walking tolerance, often needing rest after short distances
- A slowly changing posture, with her spine curving to one side
👉 Despite physiotherapy, pain relief medication, and targeted exercises, her symptoms were gradually worsening. Daily activities like gardening, shopping, or visiting friends became challenging. She was referred to a spinal specialist for further evaluation and treatment options.
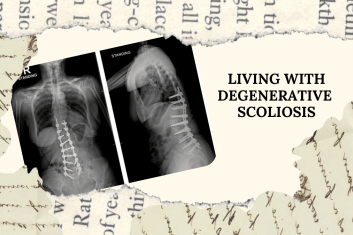
Understanding degenerative scoliosis:
Degenerative scoliosis is a condition in which the spine develops a sideways curve due to wear and tear of the discs and joints over time. Unlike scoliosis in children or adolescents, degenerative scoliosis usually develops later in life and can be accompanied by nerve compression or instability. Common features include:
- Chronic lower back pain
- Pain, tingling, or weakness in the legs if nerves are compressed
- Difficulty walking or standing for long periods
- Postural changes
👉 While imaging can look concerning, the main issue is how symptoms affect daily life. Many older adults manage well with conservative measures, but surgery may be considered when pain or reduced mobility persists
Assessment and planning:
- Mrs. X’s evaluation began with a detailed clinical and imaging assessment:
Clinical examination:
- Posture, spinal alignment, flexibility
- Muscle strength and sensation in the legs
- Walking ability and balance
Imaging studies:
- X-rays to assess the curvature and spinal alignment
- MRI scans to evaluate nerve compression and soft tissue structures
- CT scans where needed to understand bone quality and plan surgery
👉 This combination of assessments helps determine whether surgery is necessary and what type of procedure would be safest.
Modern surgical approach For Mrs.
- X, the team recommended surgery to stabilise her spine and relieve pressure on the nerves. Modern spinal surgery has evolved significantly, with several features that improve safety and recovery:
Image-guided navigation:
- Advanced imaging technology allows surgeons to place screws and implants with high precision. Think of it as a GPS for the spine — it helps avoid nerves and important structures, reducing risks.
Reduced operating times:
- With careful pre-operative planning and minimally invasive techniques where possible, surgery is performed more efficiently. Shorter operations reduce anaesthesia time, blood loss, and overall risk, especially important for older patients.
Stabilisation and decompression:
- In Mrs. X’s case, screws and rods were used to stabilise the curve, and areas of nerve compression were carefully relieved. This combination restores spinal alignment and allows nerves to recover, improving pain and function.
Recovery and rehabilitation:
- After surgery, Mrs. X spent a short period in hospital for monitoring. Key points in her recovery included:
Early mobilisation:
- She began gentle movement and walking with physiotherapy support within a day or two. Early activity helps prevent complications like stiffness, blood clots, and muscle weakness.
Structured physiotherapy:
- Exercises focused on posture, core strength, and safe spinal movement. Gradually, she regained independence in walking and daily activities.
Pain control and support:
Modern pain management strategies, including targeted medication and guidance on movement, made her recovery more comfortable and less stressful. Within a few weeks, Mrs. X noticed significant improvement in pain. Her walking tolerance increased, and she could participate in hobbies like gardening again. Her posture improved, and she reported a renewed sense of independence and confidence.
Benefits of modern surgery in older adults:
Mrs. X’s story highlights several key advantages of contemporary spinal surgery:
- Precision and safety: Image-guided navigation reduces the risk of nerve or tissue injury.
- Minimised operating time: Careful planning and efficient techniques lower anaesthetic risks.
- Faster recovery: Early mobilisation and structured physiotherapy accelerate functional improvement.
- Pain relief and mobility: Many older patients regain meaningful independence, even after years of discomfort.
- Quality of life focus: Surgery is tailored to individual goals, not just imaging results.
Key takeaways Degenerative:
scoliosis in older adults can be challenging, but modern treatment options offer real benefits:
- Early assessment is critical to determine the best approach. • Surgery is carefully planned to maximise safety, precision, and efficiency.
Recovery can be faster and more comfortable with structured rehabilitation.
Age alone is not a barrier — many older adults achieve meaningful improvements in pain, mobility, and daily life. Mrs. X’s experience shows that personalised, evidence-based care can transform quality of life, helping older patients enjoy the activities they value most.
Add a Comment