As a neurosurgeon, I have always been committed to not just removing tumors or fixing injuries, but to doing so in a way that preserves what makes each patient unique—their ability to think, speak, move, and live their lives fully. One of the most remarkable advancements in our field is awake brain surgery, a procedure that I have had the honor to perform many times. It’s a technique that embodies both precision and compassion, and it demonstrates how medicine can truly transform lives.
The Concept of Awake Brain Surgery
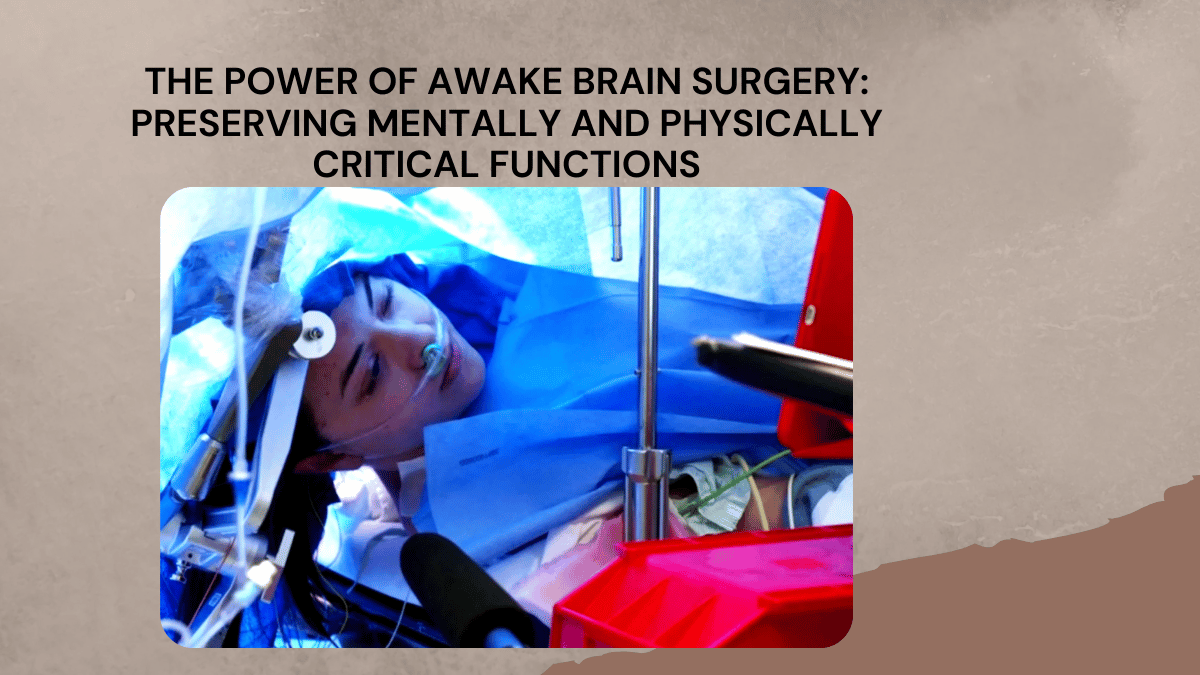
Most people think of brain surgery as a procedure done under general anesthesia, where the patient is completely unconscious. But awake brain surgery flips that idea on its head. During these surgeries, the patient is conscious, alert, and responsive. This may sound intimidating, but it’s actually quite empowering—both for the surgeon and the patient. While I operate, my team and I can monitor critical functions such as speech, movement, and sensation in real-time, making sure we are not damaging vital areas of the brain.
Why Choose Awake Surgery?
When I discuss this option with my patients, I emphasize that the goal is to remove the tumor completely while preserving their quality of life. For example, a tumor located near the brain’s language or motor centers requires extremely delicate navigation. During awake surgery, I can ask the patient to speak, count, or move specific limbs. If I notice any difficulty, I can adjust my approach immediately, reducing the risk of post-operative deficits. It’s like having the patient’s feedback as a GPS, guiding me safely through the brain’s complex landscape.
Stories of Courage and Hope
One of my most memorable cases was a young woman who had a glioma near her speech center. The tumor was threatening her ability to communicate—a critical part of her identity and livelihood. She was understandably anxious but brave. I explained that being awake during surgery would give her the best chance to keep her speech intact. As she lay comfortably on the operating table, we held her hand, and she participated actively—counting, naming objects, and talking to her family via video call. The surgery was successful, and she left the hospital with her speech preserved, grateful and full of hope.
Another case involved an elderly gentleman with a tumor pressing on his motor cortex. His family worried about paralysis or weakness. During the operation, I continuously checked his movements, and he responded quickly, enabling us to remove the tumor without impairing his mobility. His recovery was smooth, and he could continue enjoying his daily walks and hobbies. These stories remind me that awake surgery is more than just a technical feat; it’s a promise to safeguard our patients' futures.
A Blend of Skill and Compassion
Performing awake brain surgery requires immense skill, but it’s also about understanding the fears and hopes of my patients. It’s a collaborative journey—one where trust is paramount, and communication is everything. I ensure my patients are thoroughly prepared and supported every step of the way. The feeling of seeing a patient leave my operating room with their abilities preserved—that’s what makes this work profoundly meaningful.
In Conclusion
Awake brain surgery exemplifies the incredible strides neurosurgery has made, turning what was once impossible into a standard of care. For me, it reaffirms a fundamental truth: at the heart of medicine lies a commitment to preserving dignity, independence, and quality of life. Every patient has a story, and I am privileged to be part of that story—using the power of awake surgery to help write a chapter of hope and resilience.

Add a Comment