Abstract:
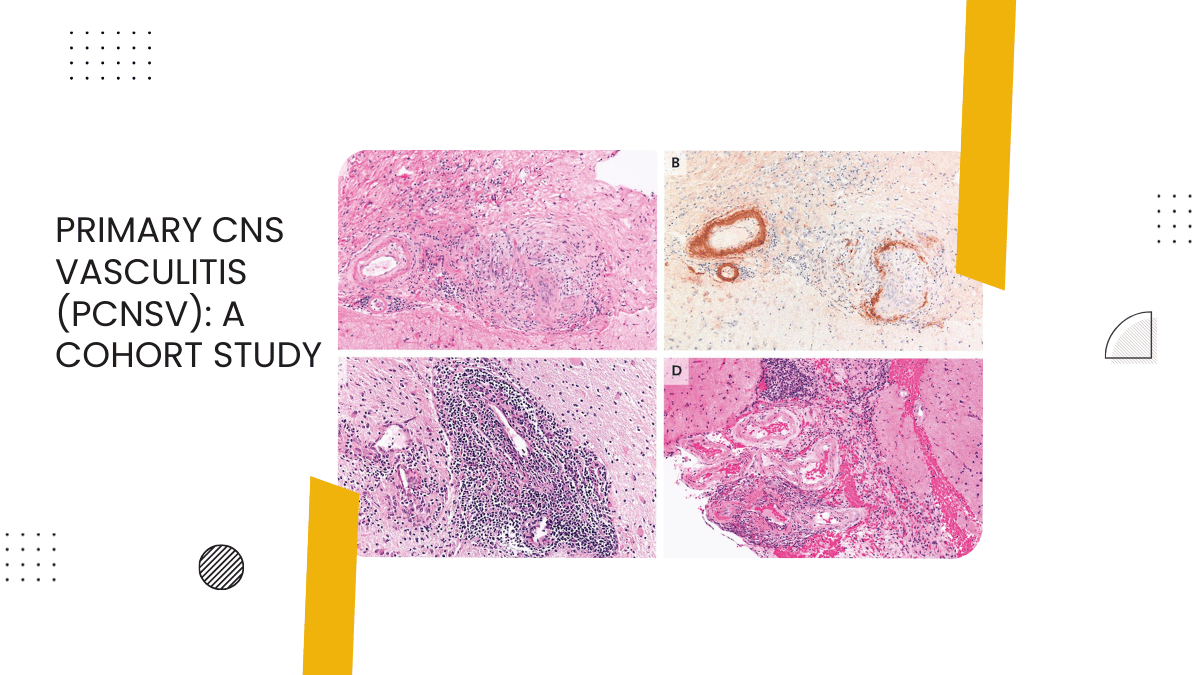
Primary CNS Vasculitis (PCNSV) is a rare inflammatory disorder affecting the blood vessels of the central nervous system. Patients present with a combination of headaches, seizures, and focal neurological deficits. There is usually a diagnostic delay. Treatment is based on observational studies and expert opinion. Our objective was to identify clinical, laboratory, neuroimaging, pathologic or management-related associations with 2 year outcome in patients with primary CNS vasculitis. We conducted a cohort study at a single tertiary care referral centre of prospectively (2018-2019) and retrospectively (2010-2018) identified individuals with primary CNS vasculitis (diagnosis was proven by either brain biopsy or cerebral digital subtraction angiography). Clinical, imaging and histopathologic findings, treatment, and functional outcomes were recorded. Univariate and stepwise multiple logistic regression were applied. P-value<0.05 was considered statistically significant. The main outcome measures were documentation of clinical improvement or worsening (defined by mRS scores) and identification of independent predictors of good functional outcome (mRS 0-2) at 2 years. We enrolled eighty-two biopsy and/or angiographically proven PCNSV cases. The median age at presentation was 34 years with a male predilection and a median diagnostic delay of 23 months. Most patients presented with seizures (70.7%). All patients had haemorrhages on MRI. Histologically lymphocytic subtype was the commonest. Corticosteroids with cyclophosphamide was the commonest medication used. The median mRS at follow-up of 2 years was 2 (0-3), and 65.2% of patients achieved a good functional outcome. Myelitis and longer duration of illness before diagnosis were associated with poorer outcomes. The presence of hemorrhages on SWI sequence of MRI might be a sensitive imaging marker. Treatment with steroids and another immunosuppressant probably reduced relapse rates in our cohort. We have described the third largest PCNSV cohort and multi-centre randomised controlled trials are required to study the relative efficacy of various immunosuppressants.
Introduction:
Primary CNS Vasculitis (PCNSV) is a rare, heterogeneous and polymorphic inflammatory disorder affecting the blood vessels of the central nervous system, often resulting in significant morbidity and mortality1,2. It has a male preponderance with a median onset of 50 years1,3,4. Patients usually present with a combination of headaches, seizures and focal neurological deficits, and there is a long time lag between symptom onset and eventual diagnosis3,4,5. The diagnosis is made by the Calabrese and Mallek criteria6, where an unexplained acquired neurological deficit with either an angiogram or CNS biopsy shows features of vasculitis, with other causes ruled out and requires a high index of suspicion.
Even though a plausible diagnosis of PCNSV may be made on MRI correlating with clinical findings and cerebral DSA, meningo-cortical/spinal cord biopsy remains the reference standard to certify the diagnosis. The treatment of PCNSV is based on retrospective studies and expert opinions since there have been no RCTs. Till date, only a few adult cohorts have been reported, the largest ones by Salvarani et al. from Mayo clinic4 and de Boysson et al. from the French cohort5. We describe the third largest cohort of adult PCNSV, including clinical demographics, management and predictors of a good functional outcome at 2 years.
To Know More Visit: https://www.nature.com/articles/s41598-022-17869-7

Add a Comment